Detect the Changes of the Cerebral Cortex Blood Perfusion of a Cardiac Arrest and Return of Spontaneous Circulation Mouse Model
System Used:
RFLSI-ZW Laser Speckle Contrast Imager

Background and Customer Needs
Cardiac arrest is the sudden termination of the cardiac ejection function, the disappearance of the great artery pulsation and heart sound, and the serious ischemia and hypoxia of vital organs (such as the brain), resulting in the termination of life. Making sure the resuscitation happens ASAP is a vital procedure to improve the survival rate. But the resuscitation also induces damage to all the organs.
After cardiac arrest (CA) and resuscitation, the unfolded protein response (UPR) is activated in various organs including the brain. The main purpose of the UPR is to restore ER homeostasis and promote cell survival. It has been well established that brain I/R insult caused by transient ischemic stroke or CA/resuscitation leads to ER stress and subsequent activation of the UPR. A previous study by this team has demonstrated that the XBP1s/HBP/O-GlcNAc axis functions in the brain and is activated after ischemic stroke or CA (6, 8). Here, the goal was to clarify the effect of this axis on functional outcomes after CA in young and aged mice.
Demand of the Research
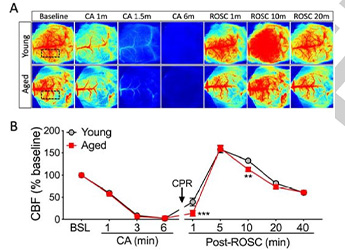
Monitor brain cortical CBF after CA in young and aged mice, to make sure the brain cortex blood perfusion changes induced by the different cardiac states show up, along with quantized perfusion data.
The blood perfusion data also can make a combination with the Glucosamine(GlcN) Western blotting, Rotarod performance, Neurologic Score, Open field and Bodyweight, and Survival Rate to figure out whether the activation of the XBP1 UPR branch in the post-CA brain is neuroprotective.
How was The System Used
In the beginning, RWD gave an online demonstration to the researchers to tell them that RFLSI Ⅲ Laser Speckle Imaging System is capable to detect the changes in the cerebral cortex blood perfusion of a Cardiac arrest (CA) and Return of spontaneous circulation (ROSC) mouse model.
Results and Effects
• CA outcome was worse in young mice with neuron-specific deletion of Xbp1 in the brain.
• CA outcome was improved in young mice with neuron-specific expression of Xbp1s in the brain.
• Short-term CA outcome in young mice was improved after post-CA treatment with glucosamine.
• Long-term CA outcome in aged mice was improved after post-CA treatment with glucosamine