(August 26, 2020) WEBINAR: Bedside to Bench: How Clinical Imaging of Patients with COVID-19 is Informing Preclinical Investigations in this Exploding Area of Research
In this webinar presented by Scintica Instrumentation, we took a look at both clinical and preclinical imaging of COVID-19. Starting with a review of current literature surrounding clinical imaging and post-mortem histological autopsy studies of patients with COVID-19, this webinar examined how these studies can inform prospective preclinical investigations using novel imaging tools to better understand COVID-19 pathophysiology.
Coronavirus disease 2019 (COVID-19), the disease caused by the novel severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has afflicted more than 20 million and killed over 750,000 individuals worldwide as of August 12, 2020 (World Health Organization).
Respiratory failure is the primary cause of disease and death in patients with COVID-19, so accordingly, chest planar x-ray and computed tomography (CT) imaging have played a large role in the management of patients in hospital emergency departments and intensive care units. CT in particular is the gold-standard clinical technique for three-dimensional imaging of lung structure and has revealed extensive lung tissue and vascular abnormalities across the spectrum of COVID-19 severity. In the most severe cases where COVID-19 causes death, select autopsy investigations have strikingly shown widespread blood clots in the lung microvasculature. Beyond lung imaging, magnetic resonance imaging (MRI) studies of the brain have also revealed drastic and heterogeneous neurological manifestations of COVID-19, including white matter and microvascular abnormalities.
 Although clinical imaging provides a window into active COVID-19 in vivo, many aspects of the pathophysiology of COVID-19 are still unclear and the rapid onset and spread of COVID-19 worldwide has made prospective clinical studies of COVID-19 impossible. This highlights the need for pre-clinical imaging of disease models to inform diagnosis and subsequent treatment of this debilitating illness. Following the discussion of current clinical imaging of COVID-19, we reviewed the pre-clinical imaging research taking place using various imaging modalities such as MRI, CT, and PET. Further we discussed the specific capabilities of these imaging modalities for prospective research projects and how the information gained from these preclinical studies may be translated into the clinical environment.
Although clinical imaging provides a window into active COVID-19 in vivo, many aspects of the pathophysiology of COVID-19 are still unclear and the rapid onset and spread of COVID-19 worldwide has made prospective clinical studies of COVID-19 impossible. This highlights the need for pre-clinical imaging of disease models to inform diagnosis and subsequent treatment of this debilitating illness. Following the discussion of current clinical imaging of COVID-19, we reviewed the pre-clinical imaging research taking place using various imaging modalities such as MRI, CT, and PET. Further we discussed the specific capabilities of these imaging modalities for prospective research projects and how the information gained from these preclinical studies may be translated into the clinical environment.
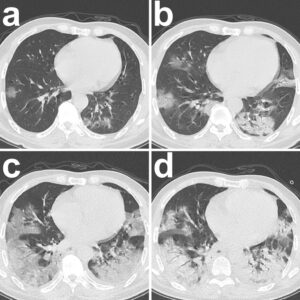
Figure caption and image taken from:
Pan, F., Zheng, C., Ye, T. et al. Different computed tomography patterns of Coronavirus Disease 2019 (COVID-19) between survivors and non-survivors. Sci Rep 10, 11336 (2020). https://doi.org/10.1038/s41598-020-68057-4

About the Speaker (s)

Patrick McCunn, PhD
Patrick McCunn is a Postdoctoral Research Fellow in Neurosciences and Mental Health at the Hospital for Sick Children in Toronto Ontario and holds a PhD in Medical Biophysics from the University of Western Ontario. His research focuses on the development and application of novel imaging techniques to detect neurodegeneration and brain injury. Additionally, Patrick works as an Applications Specialist for Scintica Instrumentation in the Imaging Division.

Rachel L Eddy, PhD
Rachel Eddy is a Postdoctoral Research Fellow in Respiratory Medicine at the University of British Columbia Centre for Heart Lung Innovation, St. Paul’s Hospital in Vancouver, British Columbia and holds a PhD in Medical Biophysics from the University of Western Ontario. Her research focuses on the development and application of novel clinical imaging tools to better understand lung disease.