Focused Ultrasound has the Potential to Improve Drug Delivery for Children with Aggressive Brain Tumours
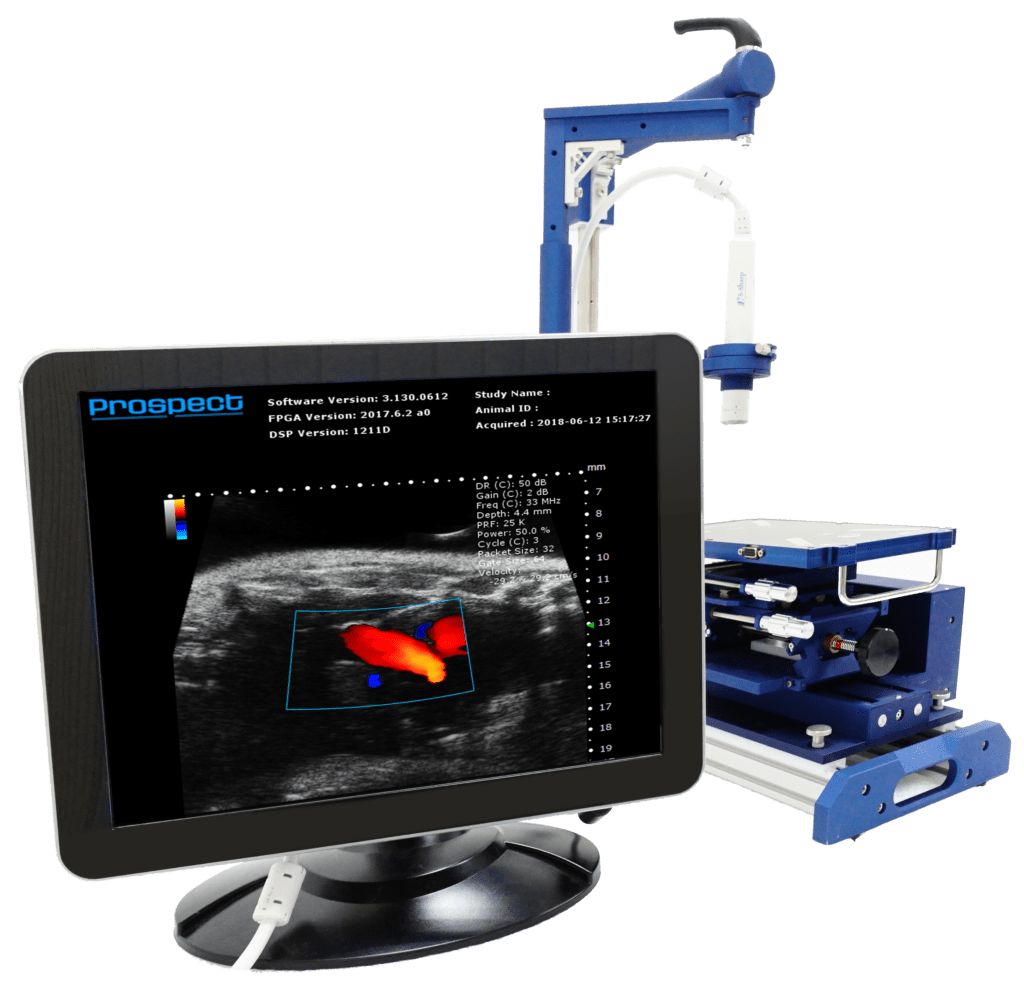
System Used:
Prospect T1
Diffuse intrinsic pontine glioma (DIPG) is a very aggressive type of childhood tumour that develops in the brainstem. Each year 200-300 children are diagnosed with the disease in North America, most commonly diagnosed between the age of 6–9 years. DIPG is the major cause of death in children with brain tumours. As DIPGs are very diffuse and infiltrate essential brain structures, surgical resection is not a viable option. Radiation therapy is the only effective treatment yet only prolongs patient life by ~3 months. Half the children with DIPG do not survive beyond 9 months after diagnosis, with only 1 in 10 children staying alive 2 years after diagnosis.
Precision medicine promises new treatments, tailored to the molecular and genetic make-up of each tumour, promising more effective and safer treatment for all children with cancer. However, like conventional chemotherapy, there is a major obstacle to the translation of these new treatments into improved outcomes in the case of children with DIPG: the blood-brain barrier (BBB). The BBB describes the unique properties of the brain microvasculature: a highly selective semipermeable border that prevents molecules in the circulating blood from non-selectively crossing into the extracellular fluid of the central nervous system. The BBB acts as a gatekeeper that protects our brain against microorganisms such as bacteria and viruses. In DIPG, the BBB remains mostly intact and, in a twisted paradox, prevents the penetration of potentially life-saving drugs into the tumors.
Recent innovations in the field of diagnostic and therapeutic ultrasound (US) have opened new avenues to improve drug delivery to brain tumours. When combined with gas-filled microbubbles, focused ultrasound has been shown to reversibly increase BBB permeability leading to a marked increase in drug delivery to the brain and the tumour. The microbubbles are US diagnostic contrast agents that can safely be injected intravenously, at the same time as the drug. Focused ultrasounds are selectively directed to the region of the brain which contains the tumour. When the microbubbles (and the drug) enter the ultrasound field, the microbubbles start oscillating volumetrically (expand and contract) causing mechanical stress and leading to the opening of the tight junctions between the cells of the BBB. This leads to increase permeability and enhanced drug penetration and distribution into the brain and the tumour. Contrast-enhanced MRI is the standard-of-care radiological measurement to assess BBB integrity (contrast enhancement is only achieved when the BBB is compromised) and was used to show proof of concept that focused ultrasound, in combination with microbubbles can transiently increase BBB permeability for both MRI contrast agent and drug in an orthotopic mouse model of DIPG.
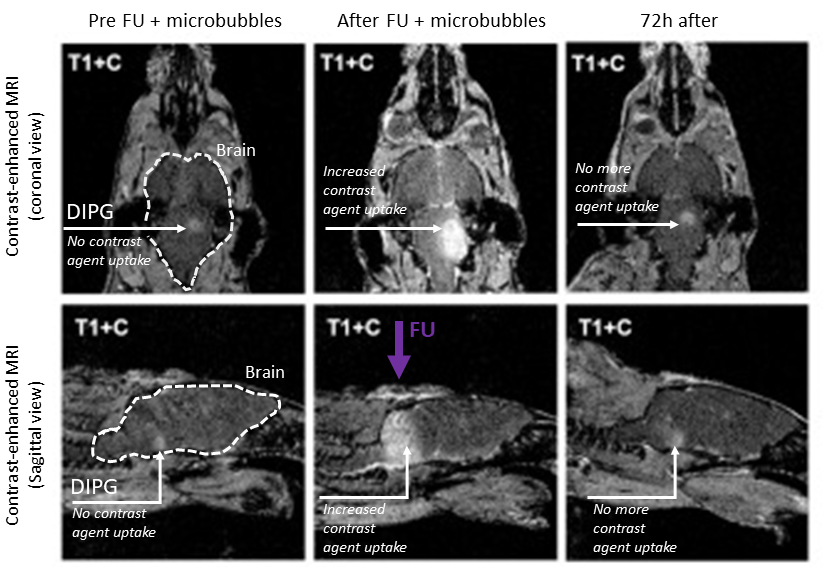
Adapted from Englander ZK et al., Sci. Rep. (2021) 11:6521
In summary, focused ultrasound provides an efficacious and safe technique to permeabilize the blood-brain barrier, a crucial step for the delivery and evaluation of desperately needed smarter and safer treatment for children with aggressive brain tumours, like DIPG.
Author
Tonya Coulthard – Manager, Imaging Division